
Growing up in India, Apoorva Mandavilli was familiar with the sight of people with leprosy—easily spotted by the characteristic limb deformities or fingerless hands—begging on the streets. The disease is a chronic, slow-progressing bacterial infection that’s plagued humans for millennia. But oddly little is known about how it spreads, and ancient myths that the deformities are a result of sin or immorality have led to people with the disease being ostracized. That stigma persists in modern society.
Thanks to global campaigns and a medication regimen that can cure infections, leprosy has largely faded from public view. Cases around the world have declined, and in 2005, the Indian government declared—prematurely—that leprosy had been eliminated. Funds from public health campaigns for leprosy were diverted to AIDS and other diseases.
So Mandavilli was surprised to learn via an email newsletter that although people assume new cases of leprosy are rare, the disease—and the stigma associated with it—persist in both rural and urban India. The newsletter blurb alerted her to a September 2018 ruling from India’s Supreme Court, which declared that the government had underestimated leprosy cases and failed to sufficiently protect patients from discrimination. The court guidelines directed the government to launch awareness campaigns, actively reduce stigma—and perhaps most importantly, do a better job of assessing the number of cases in the country, all in keeping with the World Health Organization’s goal of progress toward a “leprosy-free world” by 2020. The idea that leprosy cases were being inaccurately counted intrigued Mandavilli and led to the story “In India, a Renewed Fight Against Leprosy,” which was published April 17, 2019, in The New York Times.
Her reporting, conducted in part on an eight-day trip to visit family, took her to an urban clinic and a leprosy colony outside Hyderabad. Here, Mandavilli tells Jyoti Madhusoodanan how she found the story, how she organized and reported it, and how she framed a tightly focused tale of a country grappling with a disease no one fully understands. (This interview has been edited for length and clarity.)
How did you come across this story?
I get a newsletter from an environmental nonprofit called the Center for Science and the Environment in India because I’d written about the director, Sunita Narain, 12 years ago. In one small blurb, I saw a mention of this Supreme Court decision that was delivered in September last year, where the court was taking the government to task, saying they weren’t doing enough to prevent stigma and protect the rights of people with leprosy. They also said the government wasn’t reporting cases accurately—and that bit I found incredibly interesting. So that’s the trail I followed.
I hadn’t heard anything about leprosy in years. I started Googling and found articles about how leprosy was still a problem in India, and what exactly the Supreme Court decision was meant to combat. When I did a PubMed search, I found reviews and opinion papers where people were talking about the things that the Indian government had done wrong, so then I started calling some of those people.

Did you speak with anyone who denied that leprosy was still a problem in India?
Oh yeah—my parents. When I was on the phone with my parents discussing doing the story, my dad immediately said, “What do you mean? Leprosy isn’t a problem anymore.” And I thought, bingo!
The common perspective is that it’s gone. When I was growing up in India, you saw a lot of people with very visible deformities begging on the streets, and you don’t see much of that anymore. I think it’s better than it was before. Combined with the fact that the government wasn’t publicly talking about it anymore and there were no awareness campaigns, people really did have the sense that it was all just in the past.
Did you work with an interpreter and have to deal with their discomfort around people with leprosy?
No. Although I’ve worked with fixers before, I prefer not to work with an interpreter if I can help it. I speak multiple Indian languages, so for me, that’s one of the drives to report there as much as I can.
I think when you’re working with an interpreter you have to work so much harder at establishing that sense of trust and comfort with somebody. In this case, I was speaking to Siddamma [a key source] directly—first in Telugu, then in Kannada. We were talking about her kids, and I was telling her that I have kids the same age. It’s just a much faster path to trust with a source.
Did you have to frame your questions in specific ways to get people to talk about their experience with this stigmatized disease?
Usually I like to spend significant amounts of time with people who are going to be characters in a story. But in this case, we had two or three hours at this clinic and a lot of people we were talking to, so we didn’t have a ton of time. But I also knew this was going to be a more limited newspaper story, so I could be a little more targeted in my questions.
It also helped that these patients were at a clinic and I think they’d been told I’d be there, so they were not completely surprised. I tried to dress in clothes that look as unintimidating and natural as possible, I always make sure I wear a bindi when I’m reporting in India so that I don’t stand out. And then speaking the language goes a really long way.
Was the experience different from reporting in the U.S., where there are clear rules about confidentiality and patients’ privacy?
There’s not that same level of HIPAA protection and things like it. It’s a completely different perspective on privacy and medical details. The NGO workers were great about explaining to them why we were there and helping us connect with the patients. When I talk to patients, I always explain this is going to be in a newspaper. I find in India there’s a very basic level of literacy about journalism. They understand what it means that they’re going to be in the newspaper. They’re usually okay with that.
And people just aren’t as nervous about sharing their information. Even with things like medical records, just to illustrate—I took photos of everybody’s medical records because I wasn’t completely sure yet who I would end up writing about. And they were all okay with that. In some cases, even things like age come from the medical records because often in India you ask someone how old they are, and they’ll say things like, “Well, maybe 35. You know, you can put down whatever you want.” The doctors have their medical histories and have spent time with them to figure it out, so they have that kind of information.
That’s just to show that the people themselves don’t really care that much about exactly how old they’re supposed to be or when they were born. There isn’t that same level of attachment to information about themselves.
Do you feel like there’s more onus on you as a reporter to protect them?
I think respect has to come first. I’m always acutely aware that I want to maintain their privacy for things that aren’t relevant to the story, but also to make sure that they really understand exactly what will be used and how. I try to explain even if it seems like they don’t seem to care. I always want to make sure that they do have a sense of what it is I’m doing with them.
Also, one of the things that I always make sure they understand is that I can’t give them money. That talking to me will not end with them getting drugs, or treatment, or attention. That’s always a struggle because the rules of engagement are so defined for journalists, and yet the person on the other end doesn’t always understand that. And it can feel really uncomfortable because you know that you could so easily help them but you’re really not supposed to. Explaining that I cannot help them in those ways, that I can’t give them money and why not—that can be a little complicated. You have to be extremely conscious of not setting up expectations that they’re giving you certain information so that they can get something in return.
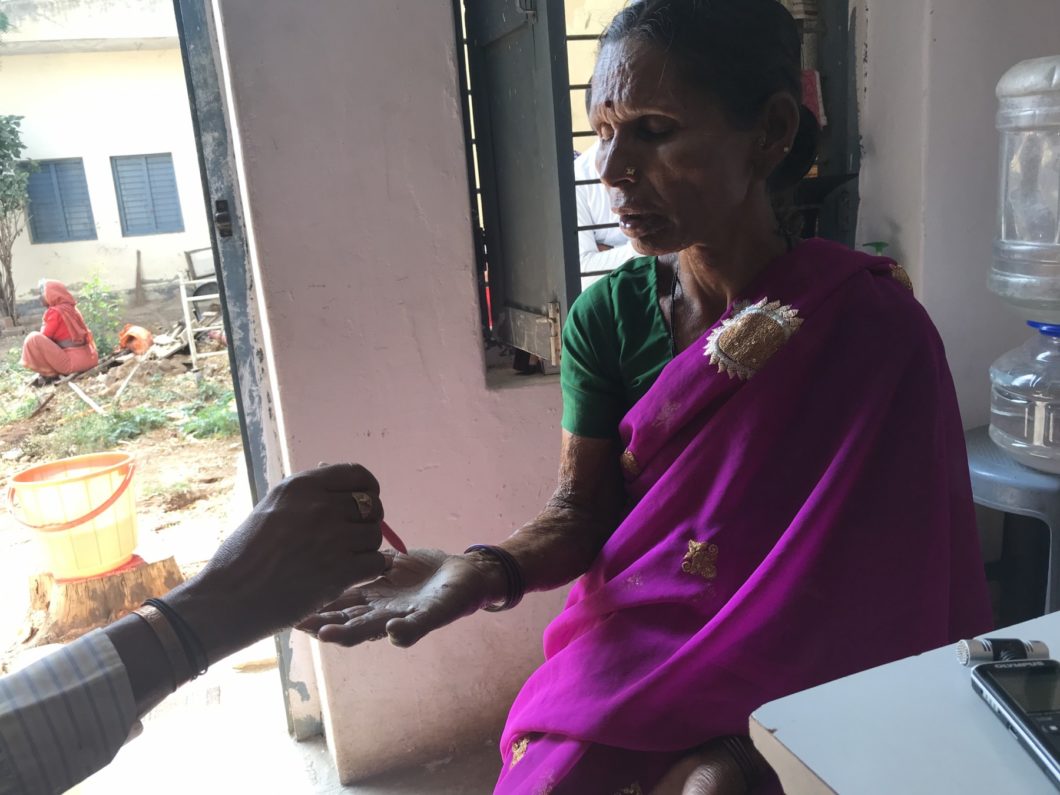
Do you have specific advice for other reporters dealing with government health officials in India?
Reaching them isn’t as complicated as it used to be since these days everyone is electronically available. I think the more difficult part is in getting them to be honest and candid about what they’re doing and why. There’s often a lot of obfuscation from Indian officials, and asking them the right questions—sometimes the tough ones—is really key. There’s more than the average level of defensiveness and hiding information.
Sometimes you have to have the information already at hand so that when they come back to you with, “Oh, but we’re doing everything we can and this is going really great,” you can immediately counter with, “Yes, but how about these numbers? If you’re doing such a great job, why have they gone up?”
Was the experience of covering leprosy somehow unique, compared to covering topics like AIDS or autism?
For me as a science journalist, there would just be moments of, “You’re kidding me.” For example, I didn’t know that the leprosy bacterium can’t be cultured in a lab, or that people don’t really know how it’s transmitted. Given that it’s such an old disease and it’s related to tuberculosis, that was a real head scratcher. There were things that cropped up during the reporting that made me aware of just how little information we have. That’s not always true for a lot of other public health problems. In those cases, you know what to do about it, but it’s just hard to get to the point of treatment, or get to the point of getting everybody services that they need. The lack of information about leprosy was really quite surprising.
I’ve often heard it’s hard to place certain global health stories because nobody cares about a few people who have this nonfatal disease in a far-flung country. Has that been your experience?

It’s absolutely true. I think there aren’t that many publications that would take a story about leprosy in India, and I’m incredibly grateful to The Times for doing it. I had the same feeling when I wrote about the Bhopal gas tragedy for The Atlantic—that nobody was going to care about that story. But it did pretty well readership-wise.
It does sometimes feel like you’re telling these very sad stories about very sad places, and who’s going to care? But I feel compelled to tell them anyway. There are just a few publications that care. And you know, it’s just a matter of convincing those particular publications and editors that the story’s worth telling.
How did you convince The New York Times to do this story?
My editor and I went back and forth a couple of times about exactly what was new in the story and how to frame it. At first, we thought maybe there needed to be new science, so I looked into drugs and vaccines, but none of that is really all that new. That’s where the WHO’s 2020 goal became the focus, because that was one of the things that seemed forward-looking.
Do you feel satisfied that you’ve told the story you wanted to, or is there more to this issue?
There are always more stories to tell. With this one, for this moment, I am temporarily satisfied. But I’d love to check back in a couple of years and see how the public health officials’ campaigns are going, whether they’re really making progress.

Jyoti Madhusoodanan is a freelance science journalist. Her work has appeared in Nature, Undark, Knowable, PBS Nova Next, and several other outlets. Find her on Twitter @smjyoti.
